
Translational model of sex differences in HF
Patients with heart failure (HF) are commonly subdivided into those with a reduced (HFrEF) and preserved (HFpEF) ejection fraction. The prevalence of HFpEF is expected to steeply increase during the following years, and will likely become the dominant HF-subtype in the near future. Prognosis of HFpEF is poor, with a mortality of 10–30% over 5 years, and burden of the disease is substantial.
Risk factors and pathophysiological processes leading to HFrEF and HFpEF differ largely: HFrEF is mostly seen in men with a history of myocardial infarction or cardiomyopathy, whereas HFpEF is a multifactorial disease expressed as several distinct phenotypes, including a common cardiometabolic phenotype characterized by obesity, type 2 diabetes mellitus (T2DM), hypertension, advanced age, and a female predominance. In contrast to HFrEF, no currently available evidence-based treatments can improve symptoms and prognosis in HFpEF patients. In addition, the development of novel treatments is hampered by the lack of animal models that can sufficiently represent the complex human HFpEF phenotype.
Laura Meems (MD,PhD) aims to improve our understanding why HF develops differently in males and females, and if these differences should translate into different treatment strategies. Her research line has a highly translational character and most of her research has a strong bench-to-bed character. Laura has recently been involved in the development of a multifactorial mouse model that resembles the human HFpEF phenotype. In this study she, and her team, were able to mimic a cardiometabolic HFpEF phenotype in old (18-22 months old) female mice. These mice developed cardiac hypertrophy and fibrosis with lung congestion, while also other comorbidities such as obesity, hypertension and impaired glucose handling were present. In this study they furthermore showed that attenuation of cardiometabolic dysregulation may represent a novel therapeutic target for the treatment of HFpEF.
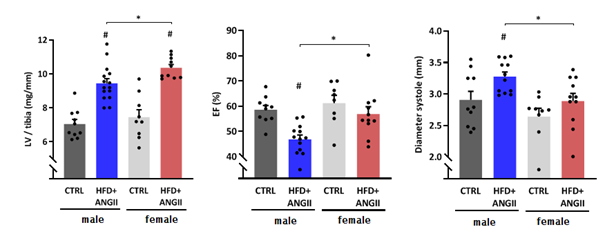
They also repeated this study in males. And albeit preliminary, they already found some interesting differences: while female mice tend to develop a more HFpEF-like phenotype, this unfavorable cardiometabolic profile results in a HFrEF-like phenotype including reduced left ventricular ejection fraction in males with increased left ventricular diameters. Ongoing studies are currently being performed to further unravel these interesting findings.
Laura recently received a Mandema grant to study sex differences further.
This is the fourth post in a series that highlights our projects related to sex differences in heart disease. A new post is published every two weeks.